- About Us
- Facilities
- Patient Stories
- Media & Events
- CSR
- Contact Us
- Book Appointment
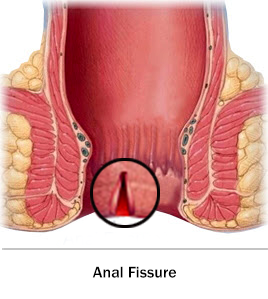
An anal fissure or Fissure-in-ano is a tear or cut in the skin of the anal canal. The condition affects men and women equally and can occur at any age ( infants too ). Anal fissures are commonly found in the back part of your anus, in line with the cleft of your buttock.
A fissure which is present for less than 6 weeks is called an Acute fissure. That which is more than 6 weeks old is called a Chronic fissure. The Chronic fissure is usually hard to feel and may have a skin tag like growth called Sentinel Pile.
Acute fissures ( < 6weeks old ) are usually treated non-surgically with medicines. Even Chronic fissures are first given a trial of medical management. The aim of the treatment is to break the vicious cycle of anal sphincter spasm and tearing of the anal skin.
At Healing Hands Clinic, Dr. Ashwin Porwal has devised a regimen called MCDPA as follows:
Sitting in warm water that covers your hips and buttocks after a bowel movement helps to reduce the post defecation discomfort.
Used in the form of an ointment, it helps to reduce spasm of the anal sphincter. However, it has side effects like headache, light-headedness which limit its role.
It is also used to relax the anal sphincter.
Acute fissures which do not heal with conservative therapy and most of the Chronic fissures need a surgical line of treatment.
The Botox is injected into the internal anal sphincter to relax it. The effects of the Botox last for 3 months by which it is hoped that the fissure would heal. However, the high cost of therapy, and a major side effect in the form of varying degrees of incontinence limit the use of Botox.
This is an age old treatment which provides good sphincter relaxation and relief from pain. However, the forceful dilatation can lead to multiple abrasions on the anal skin and may need 6-12 weeks to heal. Also, the scarred tissue over the fissure could be a source of constant discomfort and needs to be removed separately.
Done under general anaesthesia, this is a minimally invasive procedure in which a small cut is made in the internal sphincter. Thus straining during defecation is considerably reduced and there is satisfactory relief from pain. This procedures requires a good amount of skill and expertise on the part of the surgeon as an inadvertent excessive cutting of the sphincter may lead to incontinence.
This is done with the Leonardo laser introduced for the first time in India at Healing Hands Clinic. The laser is used to perform internal sphincterotomy. This procedure is almost bloodless and the surgeon has good control over the operation site. Additionally, the chronic fibrosed scar is debrided with the laser. This prevents any long term discomfort and enables a quicker recovery.
Botulinum Toxin A popularly known by brand name Botox is a neurotoxic protein that produces temporary, localized, flaccid paralysis of muscle. It is used commercially in medicine, cosmetics and research. It is often used to treat Anal Fissure, as an alternative to surgery, especially when medicines have been tried without success.
Many a times, an anal fissure is the result of an overactive sphincter muscle. This not only causes pain but also delays healing. The botulinum toxin is injected directly into the internal anal sphincter causing it to relax, thus reducing muscle tension. It also increases blood flow to the sphincter. All this aids in healing.
Painkillers may be used to relieve any pain from the injection. The effects of Botox start to become evident slowly over the next 72 hours, peak at 4 weeks and last for 3-6 months ( individual variation ). It is important to ensure that stools remain soft by taking a fiber-rich diet and stool softeners when prescribed.
Potential side effects ( seen in a minority of patients ) include bleeding, temporary loss of control over flatulence/bowel movement ( incontinence ), allergic reaction to Botox, muscle weakness and postural hypotension.
The popularity of Botox is because it offers a non-surgical option to treat chronic anal fissure. Most people have at least some relief in pain with it. It is effective in almost 60-70% cases. Another advantage is that it can be easily repeated after 6 months. There is a chance that in a small percentage of people it might not be effective and in that case other treatment options need to be considered.
A history of your symptoms followed by external inspection of the anus is enough to confirm the diagnosis.
On rare occasions your doctor may advice you other tests to rule out any suspected underlying cause for the fissure.
Fissure which is present for less than 6 weeks is called acute fissure and which is more than 6 weeks old is called chronic fissure. Both acute fissures and chronic fissures can be treated at home using medications and ayurveda therapies. But if the disease advances then surgery is required.
Laser surgery done for fissure ispainless and bloodless. Local anesthesia is given to the patient during the procedure. The post-op pain is generally cured through pain killers.
An anal fissure is a tear or cut near the anal opening. It usually heals within 3-4 weeks through simple home remedies and medications. If laser surgery is done for fissure then patient can start normal work routine from the next day of surgery and complete healing takes 1-2 weeks.
The best surgery for fissure is Laser Sphincterotomy. Laser procedure for treatment of Anal Fissure done by Leonardo Laser.
You should avoid food that leads to constipation. You should increase fluid intake and include diet rich in fiber to avoid constipation. As constipation is the main cause of fissures.
Fissures can be healed through some lifestyle modifications and medications. Lifestyle modification includes physical activities, having enough fluids and fiber rich diet. Sitting in warm water after bowel movement also helps to reduce discomfort