A fistula is a painful and persistent medical condition that can significantly affect your quality of life. It occurs when an abnormal tunnel forms between two organs or between an organ and the skin. One of the most common and troublesome types is the anal fistula, which typically develops due to an infection in the anal glands. If left untreated, a fistula can cause recurrent abscesses, discharge, pain, and infection. Fortunately, fistula treatment in Hyderabad has become more advanced, with skilled surgeons and modern techniques offering long-lasting relief.
In this blog, we’ll explore everything you need to know about fistula treatment in Hyderabad — from symptoms and causes to treatment options and choosing the best fistula doctor in Hyderabad.
What is a Fistula?
A fistula is an abnormal connection between two body parts. In the case of an anal fistula, the tunnel forms between the anal canal and the skin near the anus. It usually develops after an anal abscess fails to heal completely and leaves a tunnel behind.
Symptoms of Anal Fistula
If you’re experiencing any of the following symptoms, it’s essential to consult a fistula specialist doctor in Hyderabad:
- Constant or recurring pain near the anus
- Swelling or redness around the anal area
- Pus or blood discharge
- Itching or irritation
- Fever due to infection
- Pain while passing stools
Causes of Anal Fistula
The most common cause of an anal fistula is an infection in the anal glands. Other contributing factors include:
- Crohn’s disease (an inflammatory bowel condition)
- Trauma or injury to the area
- Surgery complications
- Tuberculosis or sexually transmitted diseases (rarely)
- Chronic constipation or diarrhea
Getting an accurate diagnosis is essential for effective treatment. A qualified anal fistula doctor in Hyderabad will perform a physical examination and may suggest diagnostic tests like:
- MRI scan or ultrasound
- Anoscopy
- Fistulogram
These tests help the doctor determine the exact location and complexity of the fistula, which is crucial in selecting the appropriate treatment method.
Treatment Options for Fistula
Fortunately, advancements in medical technology have made fistula treatment in Hyderabad safer and more effective than ever. Depending on the type and severity of your fistula, the doctor may suggest one of the following:
1. Fistulotomy
This is the most common surgical procedure for simple fistulas, where the fistula tract is cut open and allowed to heal from the inside out.
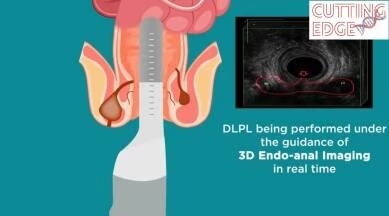
2. Laser Surgery for Fistula
Laser surgery is a minimally invasive technique with faster recovery and less pain. It’s an excellent option for patients seeking a more comfortable treatment experience.
3. LIFT Procedure (Ligation of Intersphincteric Fistula Tract)
Ideal for complex fistulas, this procedure preserves the anal sphincter and reduces the risk of incontinence.
4. Seton Technique
Used for high-risk or recurrent fistulas, a seton (a surgical thread) is placed to allow the fistula to drain while slowly healing.
Why Choose Hyderabad for Fistula Treatment?
Hyderabad is known for its advanced healthcare facilities and experienced medical professionals. Whether you are looking for a fistula surgeon in Hyderabad or a best lady fistula doctor in Hyderabad, the city offers plenty of trusted options with a proven track record.
Moreover, modern hospitals and proctology clinics in Hyderabad now provide access to painless laser treatments, skilled post-operative care, and minimal downtime — making it easier for patients to recover quickly.
Finding the Best Fistula Doctor in Hyderabad
When choosing a fistula specialist doctor in Hyderabad, consider the following factors:
- Experience and Expertise : Look for doctors who specialize in proctology and have extensive experience in treating fistulas.
- Advanced Treatment Options: Ensure the clinic offers modern techniques such as laser treatment.
- Patient Reviews: Check patient testimonials and success stories to gauge the doctor’s credibility.
- Hospital Facilities: Opt for a well-equipped hospital with advanced diagnostic and surgical tools
Dr. G. Uday Kiran: Leading the Way in Surgical Excellence at Healing Hands Clinic, Hyderabad
In the world of modern healthcare, few doctors combine expertise, compassion, and innovation as seamlessly as Dr. G. Uday Kiran. With over a decade of experience in Laser Proctology, General Surgery, Minimal Access Surgery, Laparoscopic Procedures, and Gynaecological Interventions, Dr. Kiran is a dedicated proctologist and surgeon who is committed to providing the best possible care to his patients. His passion for advancing medical science ensures that each patient receives the most effective and least invasive treatments available.
Dr. Balakrishna Pitike: A Trusted Name at Healing Hands Clinic, Hyderabad
Dr. Balakrishna Pitike is a dedicated and skilled proctologist, renowned for his expertise in anorectal diseases and his compassionate approach to patient care. A young and passionate professional, he has received numerous positive reviews from the patients he has treated, showcasing his commitment to exceptional surgical outcomes and patient satisfaction.
Dr. Vismaya M: A Compassionate and Skilled Proctologist Dedicated to Women’s Health
Dr. Vismaya M is a highly respected surgeon and proctologist known for her proficiency in treating anorectal conditions with minimal invasive procedures. With a passion for women’s health, she has earned a reputation for her compassionate care, strong interpersonal skills, and dedication to continuous professional development. Dr. Vismaya is deeply committed to making her patients feel comfortable and confident in addressing sensitive health issues that many women shy away from discussing.
Healing Hands Clinic – A Trusted Name in Fistula Care
One of the leading proctology centers offering fistula treatment in Hyderabad is Healing Hands Clinic. Known for its expertise in minimally invasive procedures like laser surgery for fistula, the clinic has helped thousands of patients recover from this painful condition. The team of fistula specialist doctors in Hyderabad ensures a comprehensive and personalized approach to care — from diagnosis to postoperative follow-up.
Final Thoughts
Living with a fistula can be frustrating and painful, but you don’t have to suffer in silence. With modern treatment options and expert care from the best fistula doctors in Hyderabad, long-term relief is absolutely possible. Whether you’re looking for advanced laser treatments or experienced surgeons, Hyderabad offers comprehensive solutions tailored to your needs.